MOBILITY DEVICES & CUSTOM SUPPORT
The right device for your pet isn't always the one you came in asking about. Sometimes it's exactly that. We'll help you find out which.

Whether you were referred here with a specific recommendation, sent by a vet who knows what we do, or you've been researching on your own and aren't sure what your pet needs — this is the right place to start. We assess before we prescribe. Always.
HOW WE THINK ABOUT DEVICES
A device is a tool. The animal is the patient.
Mobility devices can be genuinely life-changing. A well-fitted wheelchair returns independence to a dog who lost the use of their hindlimbs. A properly prescribed brace stabilizes a joint while the surrounding musculature rebuilds. A prosthetic limb restores not just function but something harder to measure: the animal's relationship with their own body.
The device doesn't do any of that on its own.
What makes the difference is fit: precise, iterative, supervised fit that accounts for your pet's specific anatomy, diagnosis, neurological status, movement patterns, and how all of those change over time. A device that isn't fitted correctly doesn't just fail to help. It can actively create new problems: pressure sores, compensatory injuries in healthy limbs, gait alterations that load the spine in ways that compound the original issue.
A mobility device is not a prescription you fill once. It's a practice you build.
That framing shapes everything we do here.
Fitting is a process, not an event. We make adjustments at the first fitting. We make more adjustments as your pet adapts. We make further adjustments as their condition evolves, sometimes toward greater function, sometimes in response to a setback that requires us to recalibrate.
Adam's background in construction and fabrication means we don't stop at what the manufacturer provides. We modify, pad, reinforce, and customize using whatever the situation calls for. Dr. Heather's clinical assessment ensures that every modification is grounded in what the anatomy actually needs, not just what fits on paper.
One practical reality that surprises most people: mobility devices require supervision during use. A dog in a wheelchair who tips over and can't right themselves may be stuck in that position for a long time if no one is watching. A pet who won't tolerate a prosthetic may damage both the device and their residual limb trying to remove it. A brace that shifts during activity changes the load profile of the joint in ways that can worsen the problem it was meant to solve.
This isn't a reason to avoid devices. It's a reason to use them with eyes open, and with someone in your corner who knows what to watch for.
SOMETIMES THE HIGHEST RETURN ON YOUR INVESTMENT IS ELSEWHERE
Reducing the load the body is working against.
The body heals in an environment. When that environment is chronically inflamed, poorly nourished, or sleep-disrupted, the ceiling on recovery is lower than it needs to be.
Nutrition is directly tied to mobility outcomes, not in a supplement-as-magic-bullet sense, but because systemic inflammation affects tissue quality, joint health, pain regulation, and the nervous system's capacity to adapt. We look at what the cells are working with: the building blocks available for tissue repair, the inflammatory load the system is managing, the quality of the environment in which recovery is being asked to happen.
Circadian rhythm matters more than most owners realize. Sleep is when tissue repairs and the nervous system consolidates motor learning. Consistent schedules, light exposure, and attention to the rest environment can meaningfully shift the baseline.
Olfactory enrichment, time outside at nose-pace, following scent, processing the environment through smell, is not a soft addition to a rehabilitation plan. It is direct input into nervous system regulation, stress reduction, and cognitive engagement, all of which have measurable downstream effects on pain experience and recovery capacity. A dog who spends an hour on what we call a snifari is doing rehabilitation. The research on this is real, even if it doesn't always make it into discharge instructions.
Building the body that can use a device well — or not need one.
Core strength and movement vocabulary are the foundation of everything we do. A dog with strong stabilizing musculature, good proprioceptive awareness, and a varied movement diet is a fundamentally different patient than one whose world has narrowed to couch-to-yard-to-couch.
Proprioceptive awareness is the body's continuous sense of where it is in space: how much load each limb is bearing, and how to adjust in real time. When that system is disrupted by injury, surgery, or neurological compromise, a pet doesn't just lose strength. They lose confidence in their own movement, the deep automatic trust that a limb will do what they ask of it. Rebuilding that trust is as much a neurological project as a physical one. It responds well to targeted, progressive exercises that most owners can develop genuine skill at delivering at home.
This matters because the work that happens between appointments, in your living room, on your walk, in the backyard, is where recovery actually lives. We give you the tools. You build the practice. We refine it together.
The best version of your pet may not need a device at all.
This isn't a way of talking you out of something you came here for. It's an honest accounting of what assessment sometimes reveals: a meaningful number of pets referred to us for mobility devices have more to gain, at this moment, from a different kind of investment. Sometimes a device becomes indicated later. Sometimes the work we do together makes it unnecessary. Either way, the assessment tells us, and we tell you.
When we find that a pet's time and capacity are better spent elsewhere first, here's what that typically looks like.
Finding the level you can actually sustain.
The best plan is the one that gets executed. We don't optimize for the maximum possible intervention. We optimize for the maximum sustainable one. That means understanding your schedule, your capacity, your pet's tolerance, and what enough actually looks like in your specific situation.
Some people want a focused home exercise program and clear checkpoints. Others want to go granular: tracking progressions, logging observations, building their own reference that we review and respond to. Both approaches work. We find the level that gives you enough to act on without overwhelming the system, yours or your pet's, and we build from there.
"The most overlooked investment in a pet's health isn't a treatment or a device. It's the quality of how they move every day.
A body that moves well, with strength, coordination, and real confidence in its own limbs, is more resilient, heals faster, and ages better. We're talking about the whole system: muscle, fascia, the circulatory system, the nervous system, the environment the cells are living in. When that system is well-built, it handles the hard events better. Surgery is less catastrophic. Recovery is faster. The bad days are less bad.
Most people don't think about this until something goes wrong. We try to get there first, and to bring you with us."
— Adam Yoshida, CSCC · Integrative Health Coach
WHAT WE WORK WITH
The tools — and what working with them actually requires.
A note before we go through the devices.
Every mobility device on this list asks something of the caregiver, not just the pet. Bending to support a large dog. Navigating stairs while managing a harness. Walking backwards through an exercise pattern with your attention on the animal instead of where you're stepping.
These are physical demands, and we pay attention to them. Not because we assume you can't handle them, but because identifying risks before they become problems is part of how we think. When we walk you through device use and home exercise protocols, we look at what it asks of your body too. Sometimes awareness is enough. Sometimes there are adjustments we can make that protect your posture and movement before anything becomes an issue.
If the caregiver goes down, so does the pet. We take that seriously from the first appointment.
Harnesses and slings provide targeted lift and support for pets with weakness, balance issues, or post-surgical mobility limitations. Used well, they assist just enough: supporting the animal while allowing them to bear as much healthy weight as possible, building rather than bypassing the strength we're trying to rebuild.
The Help 'Em Up Harness, which we use most, is highly customizable. Multiple strap points across the shoulders and hips all require precise trimming and adjustment to get the most out of the device for your specific pet. We handle fit at the appointment, walk you through application until it's second nature, and remain available as questions come up.
For owners providing daily physical support to a larger dog, getting this right matters. The difference between a properly fitted harness and improvised support is the difference between a sustainable caregiving practice and one that creates its own problems over time.
Harnesses and slings — for assisted movement with intention.
A wheelchair is indicated when a pet has lost meaningful use of their hindlimbs and the prognosis or owner preference makes long-term mechanical support the right path. Device selection depends on a clinical read of your pet's specific presentation: their diagnosis, neurological status, body geometry, and trajectory. A pet who presents one way today may change significantly over weeks of treatment, and the right device for week one may not be the right device for week six.
We have experience fitting and modifying wheelchairs across multiple manufacturers and choose based on where the patient is right now and where we expect them to go. What most people don't anticipate is the fitting process, the training process, and the supervision requirements. A well-fitted wheelchair returns genuine freedom and joy. Getting there takes more than unboxing.
Wheelchairs — for hindlimb paralysis, severe weakness, or balance deficits.
Carpal braces, hock braces, stifle orthotics: powerful tools when correctly indicated, properly fitted, and used as part of a rehabilitation plan. Custom braces are available direct to consumer, but no patient should be wearing a device that restricts range of motion without a rehabilitation professional overseeing case selection, device selection, and fit. What's appropriate depends entirely on the specific patient, the specific diagnosis, and the specific goals, and that determination requires clinical expertise.
We provide the clinical prescription, the hands-on fitting, and the follow-up adjustments as the situation evolves. The device and the rehabilitation plan work together. One without the other is incomplete.
Braces and orthotic devices — for joint stabilization within a rehabilitation plan.
Traction and grip solutions address a specific and underappreciated problem: the pet who has the neurological intent to move but can't maintain contact confidence with the ground. Which solution fits depends on the patient's clinical picture, their home environment, and what their movement goals require. The options have meaningfully different tradeoff profiles.
Nail-applied grips restore traction without restricting movement or requiring daily application. Tolerance varies by patient, and we assess candidacy before you invest. Adhesive traction pads applied directly to the foot pad offer an alternative for pets who won't accept nail-applied options: different demands, different situations where they work well.
Booties protect the foot and add traction, and for some situations, preventing scraping or abrasion in pets who drag their toes or can't fully return the foot to normal position before ground contact, they earn their place. The tradeoff is proprioception. A boot dampens the sensory feedback between foot and ground: the continuous conversation that tells the nervous system where the limb is and how to adjust. Whether that tradeoff is worth it depends on what you're trying to accomplish. We help you think that through before you invest.
Traction and grip devices — where the rubber meets the road.
Some pets, particularly those with neurological deficits, have difficulty with normal foot strike. Instead of the bottom of the foot contacting the ground first, the top of the foot makes contact. This is called knuckling, and it creates two problems: injury to the top of the foot over time, and a gait pattern that compounds neurological and biomechanical dysfunction.
Toe-up devices create a light assist that encourages the foot back into proper position during the swing phase of walking, so that when the foot lands, it lands correctly. In some cases, a bootie serves as the platform for a toe-up device, combining protection and mechanical correction in one system.
Whether a toe-up device is indicated, which type, and how it interacts with any other devices in use are conversations we have directly with you, based on what we observe. We set you up knowing what to watch for and when to come back so we can adjust as your pet's situation evolves.
Toe-up devices — for pets who need help returning their foot to normal position.
Prosthetics can restore a quality of movement, and a quality of life, that surprises everyone who assumed the ceiling was lower. Experience with prosthetic fitting is rare even among rehabilitation practitioners. We have it, and it has taught us things no manufacturer's guide covers.
Cleo, one of our long-term patients, has been in a prosthetic for years. Her device worked well. Her body has changed over time: she's aged, gotten stronger in some areas, and developed new needs in others. Her prosthetic situation has evolved with her. That's not a complication. It's a body doing what bodies do. The response is what it's always been: ongoing assessment, honest iteration, and a rehabilitation foundation that has kept her stronger and more capable throughout. We're currently evaluating next-generation 3D-printed options that offer advances in fit precision for patients whose needs have outpaced what earlier manufacturing could provide.
Success with a prosthetic comes down to two things: the owner's investment in the process, and the quality of rehabilitation surrounding the device. We manage the complete process, from assessment and measurement through casting, fitting, and rehabilitation, in partnership with qualified prosthetic manufacturers. We won't promise a trajectory we can't see yet. We will build the foundation that gives any prosthetic its best possible chance, and adapt honestly when the situation calls for it.
Prosthetic devices — for limb loss, with realistic expectations and serious rehabilitation.
WHAT WORKING WITH US LOOKS LIKE
Assessment first. Device second. Iteration throughout.
Every device engagement starts the same way: we look at what's actually happening before we reach for a solution. Dr. Heather conducts a full physical and neurological assessment. We review your records. We watch your pet move. We ask you what you've noticed at home, because your observations are clinical data.
From that assessment, we determine whether a device is indicated, which device category makes sense, and what the fitting and use plan looks like. In many cases, we identify parallel work: rehabilitation exercises, home practice, environmental modifications that run alongside the device and determine how much the device ultimately has to do.
After fitting, we teach. Application technique, wearing schedule, what to watch for, when to contact us. You leave knowing how to use what you have.
Then we follow up. Devices are not set-and-forget. We make adjustments as your pet adapts, as their condition evolves, and as you both develop skill and confidence with the tool.
A fitting in three steps.
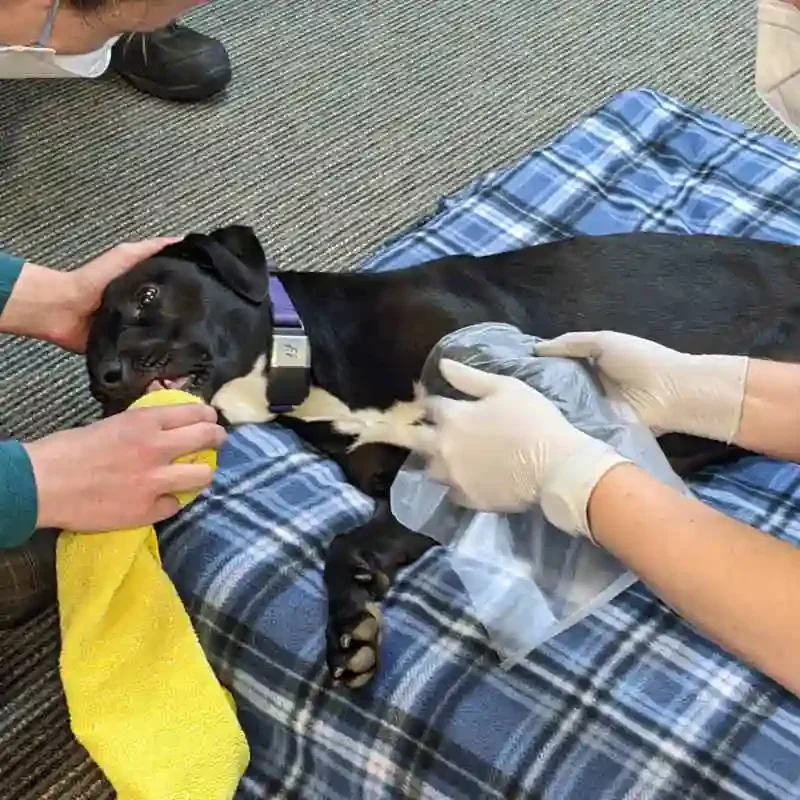
Step 1: Casting the affected limb for precise measurement.
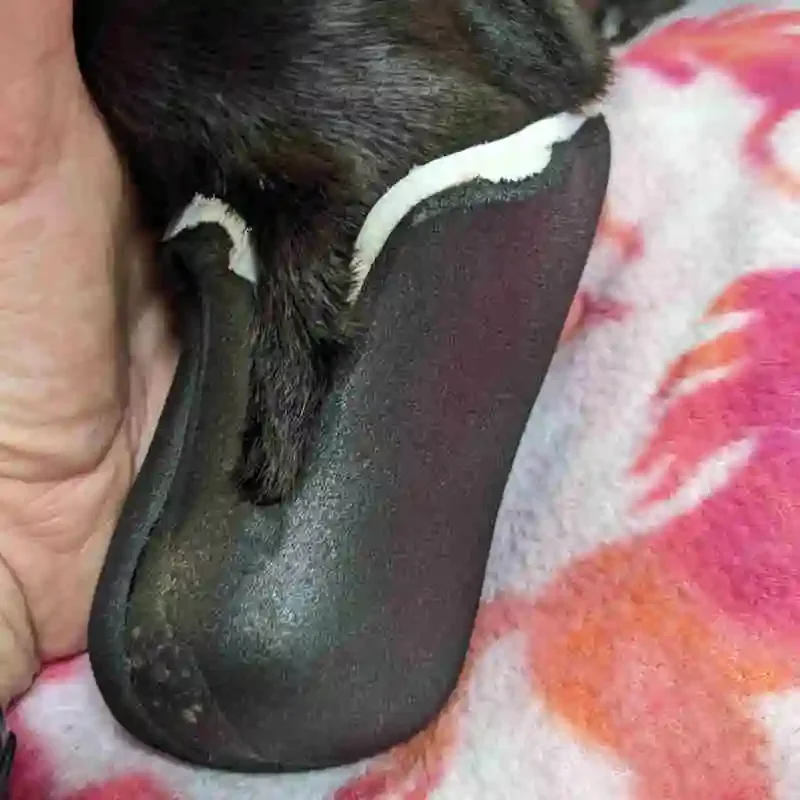
Step 2: Fitting the foam insert to the residual limb.

Step 3: First fitting of the completed prosthetic — and the beginning of breaking it in.
The process doesn't end at step three. It's where the rehabilitation work begins.
Not sure if a device is what your pet needs?
That's exactly the right question to bring us.
Our initial consultation is 75 minutes. We review your records before you arrive. We assess, we listen, and we tell you what we actually find — including when the answer is something other than what you came in expecting.
Questions first? hello@ruffday.vet
Stories of Transformation & Resilience
The true measure of our impact lies in the lives we've transformed and the peace of mind we bring to pet parents.
Explore compelling testimonials and success stories from other families who have partnered with Ruff Day Vet + Pet Gym.
Empower Your Pet's Health: In-Depth Articles & Resources
Understanding your pet's health can be a journey, and we're here to guide you. The Ruff Writer blog provides a deep dive into integrative veterinary medicine, offering detailed articles, essential resources, and our unique perspectives.
We aim to contribute to a thoughtful discourse, continually expanding the body of knowledge available to you as a pet owner.






What if we treated our business operations the same way we treat rehabilitation patients - observe, ask questions, iterate, improve? We tried redirecting our marketing budget from ad platforms to local charities. Here's what happened in Year 1 of this active experiment.